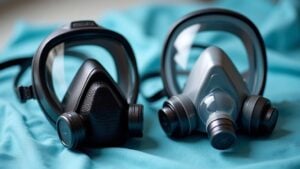
As you’re faced with selecting between a rebreather and nonrebreather mask, comprehension of their differences can make all the difference in patient care. You may question why one provides higher oxygen levels or how valves play a role in airflow control. Each has specific clinical uses, from emergencies to stable conditions, and safety checks are vital for both. Recognizing these distinctions guarantees you pick the right tool—but which one fits your situation best? Let’s break it down.
Oxygen Delivery Mechanism
At the moment you need quick oxygen support, non-rebreather and rebreather masks work differently to get oxygen into your system.
A non-rebreather mask uses one-way valves to keep exhaled air from mixing with fresh oxygen, boosting oxygen concentration to 60-90%. It fills a reservoir bag with pure oxygen, ensuring high concentrations of oxygen reach you quickly—perfect for emergency situations. The oxygen flow rate stays high (10-15 liters per minute) to keep the bag inflated.
A partial rebreather mask, however, lets some exhaled air back into the reservoir, lowering oxygen delivery to 40-60%. It’s less efficient for short-term use but still helps when high flow isn’t critical.
Both rely on their design to control oxygen delivery, but one prioritizes speed and purity.
Valve System and Airflow Control
Whenever you’re relying on a mask for oxygen, the way airflow is managed makes all the difference.
A non-rebreather mask uses one-way valves to block exhaled air from mixing back into the reservoir bag, keeping oxygen concentration high—ideal for severe hypoxemia.
The partial rebreather mask, though, has a two-way valve that lets some exhaled air recycle, lowering oxygen levels but adding humidity.
Flow rates for both masks are similar (12-15 L/min), but the non-rebreather’s tight valve system guarantees purer oxygen by preventing room air from diluting the supply.
Should you need maximum oxygen, the non-rebreather’s design wins.
But in cases where humidity matters more than concentration, the partial rebreather’s airflow control may suit you better.
The valve system decides what you breathe—so choose wisely.
Oxygen Concentration Levels
Since oxygen concentration levels determine how effectively address breathing difficulties, it’s essential to understand the differences between mask types.
A non-rebreather mask delivers high oxygen levels (60-90% FiO2) by preventing exhaled air from mixing with fresh oxygen, making it ideal for emergencies. In contrast, a partial rebreather mask allows some exhaled air to recycle, lowering oxygen delivery to 40-60%.
The flow rate matters too—non-rebreathers need 12-15 L/min to keep the reservoir bag full, while partial rebreathers use 10-15 L/min but sacrifice mask effectiveness due to air mixing.
Should you require rapid, high-concentration oxygen, a non-rebreather wins. For milder cases, a partial rebreather balances comfort and oxygen levels. Always match the mask to the patient’s needs for the best results.
Clinical Use Cases
While you’re facing a breathing emergency, the right oxygen mask can make all the difference—non-rebreather masks (NRMs) step in while every second counts. They deliver high-concentration oxygen (60-90% FiO2) for life-threatening cases like carbon monoxide poisoning or severe lung injuries.
In an acute care facility, NRMs are your go-to for rapid oxygen therapy as blood oxygen levels plummet dangerously low. They’re also used for COPD flare-ups or cluster headaches, where quick critical intervention is essential.
Partial rebreather masks, on the other hand, suit less urgent needs, offering lower oxygen concentration (40-60% FiO2) by letting you rebreathe some exhaled air.
Providers must monitor patients closely to guarantee the oxygen supply doesn’t run out and the mask functions properly.
Choose wisely—your breath depends on it.
Patient Safety and Monitoring Requirements
Because every breath matters, keeping an eye on safety and monitoring while using oxygen masks isn’t just essential—it’s a lifeline.
With a non-rebreather mask, one-way valves block exhaled air, ensuring you get a high concentration of oxygen without mixing in stale breaths.
But this also means you need tight monitoring requirements—check the reservoir bag stays inflated and the flow rate stays at 12-15 liters per minute.
Should it fail, your oxygen delivery drops fast, risking respiratory distress.
Unlike rebreathers, where exhaled air can dilute FiO2 delivery, the non-rebreather’s design demands constant attention.
Watch for mask leaks, tank levels, and signs of discomfort.
Your patient safety hinges on these details, so stay alert—every second counts when breathing’s on the line.